My phone rings Thursday, December 1st, at 6 pm. It's the nurse practitioner calling from the rheumatology office. She's calling to inform me that our follow-up appointment is scheduled for January 9th. In the meantime, we should start rituximab for our daughter's refractory thrombocytopenia.
Our initial visit was on November 7th with Dr. "X" (we'll keep her anonymous). That's two months between the first and second visit. That's two months of waiting for answers.
Two weeks prior, I was in a very dark place as I saw lab results coming in one-by-one.
I started to think about every possible outcome for my daughter's life. Everything from living an inconveniencing life to death. Each abnormal lab result sent me down a different road of possibilities.
I pictured a lifetime of blood work, medications, and hospital admissions. I saw the sadness on my daughter's face. I saw the hurt in her eyes. I was in tears for two full days as I fell victim to my imagination.
Having a medical background can be a double-edged sword. On the one hand, you can question the "authority" of the white coat when something sounds off. But it also means you're aware of what can happen to the one percent of patients (this isn't always helpful).
Because it's my daughter, I held that focus on what could happen. Not what was most likely to happen.
When Chloe was seven months old, I shared concerns about systemic lupus erythematosus (SLE). I noticed a malar rash and brought it to our pediatrician's attention. But, he told us it didn't have the classic appearance and was unlikely to be from SLE.
As we continue our quest, I can't help but wonder why we dismiss specific atypical findings when she's been an atypical case from the start.
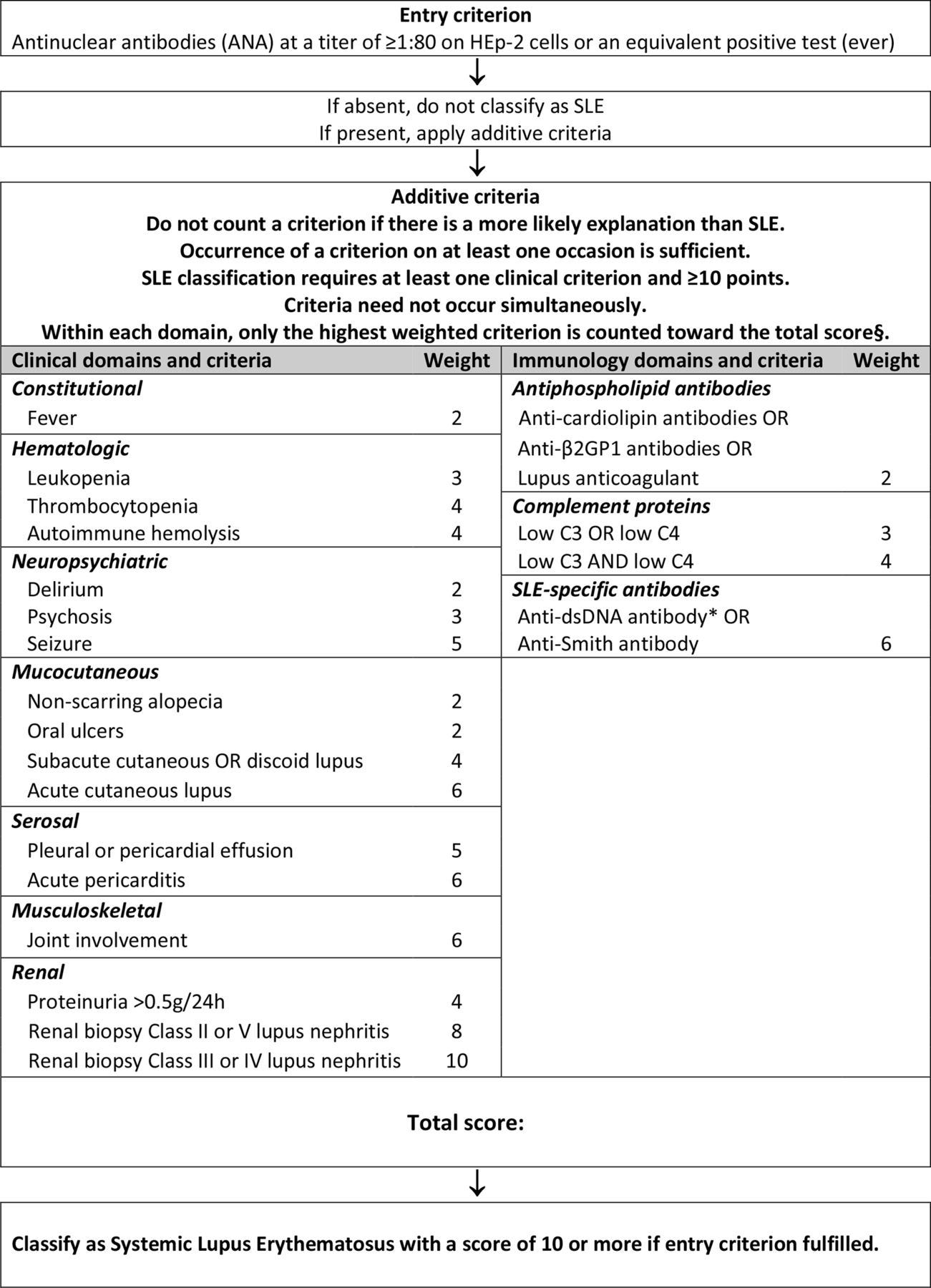
Let's take a break from the emotional aspect of things to discuss a little medicine. Our rheumatologist uses the 2019 EULAR/ACR Classification Criteria for Systemic Lupus Erythematosus.
This criterion requires an ANA at a titer of ≥1:80 on HEp-2 cells to consider SLE a possible diagnosis. If the ANA is negative, we cannot classify a patient with SLE, and the workup stops here. If the ANA titer is ≥1:80, we may look for the additive criterion to be met: one clinical and a score of ≥10 points.
Chloe had an ANA titer of 1:40 on HEp-2 cells and a score of 17 points:
Thrombocytopenia: 4 points
Oral ulcers: 2 points
For argument's sake, I've excluded the malar rash and other skin manifestations.
Positive anti-B2GP1 antibody: 2 points
Low C3: 3 points
Positive anti-dsDNA antibody: 6 points
We can be even more conservative and remove the oral ulcers, as I noticed them on the gingivae, and classically they are seen on the hard palate.
This would give her a revised score of 15, which is well over the minimum threshold of 10.
Although Chloe meets the scoring criteria, they are reluctant to call this lupus because she had a weakly positive ANA titer. This logic would make sense if the ANA were 100% sensitive, but it's not.
It is hard to believe that we require a lab value that we know isn't present in 100% of patients ultimately diagnosed with SLE. Requiring the ANA as an entry serves well for 98% of cases and will prevent overdiagnosing. This is perfect for clinical trials and looking through a lens of statistics where we can help the majority. This is not great when you are part of the 2%.
More importantly, the ANA may be negative in the early stages of this disease when identification is critical to preventing organ damage.
To confuse matters further, this criteria's original sensitivity and specificity were based on a cohort of 2,271 patients aged 31 - 72. The 2019 EULAR/ACR criterion has yet to be validated in the pediatric population since being peer-reviewed and published. There have only been retrospective studies, but these show conflicting results regarding the sensitivity and specificity of the criterion in children.
My daughter is only one year old.
Even in the retrospective studies, the children were older, as it's rare for lupus to be diagnosed in patients under five, further limiting the utility of the scoring criteria. One could argue that lupus is seen in patients under 5, but they get dismissed because it's not severe (yet). Then, years later, when signs of end-organ damage occur, they are finally diagnosed.
Unfortunately, we'll never know if this is the case; I hope it’s not. In any event, I had questions and concerns I was hoping to bring up to our rheumatologist:
The ANA came back with a speckled appearance. When done with an automated immunofluorescence test, speckled patterns may lead to a false negative ANA or falsely low ANA titer.
ANA titers are just a snapshot in time. ANA titers may be low at the onset of the disease and increase over time. Keeping that in mind, it's well established that titer levels don't correlate with severity.
Similarly, we need to remember that there is normal testing precision variability. In other words, the titer can go from 1:40 -> 1:80 because of inherent variability with the lab, not necessarily because there's a change in the disease state. This is partly why titer levels don’t correlate with the severity of the disease.
If you saw my last post, you'll notice Chloe had a positive anti-dsDNA which increases the likelihood that she has a true positive ANA. But, I've seen false positives for anti-dsDNA occur if the test was done via ELISA (which it was). A repeat test with Crithidia luciliae indirect immunofluorescence test (CLIFT) has been recommended to confirm a true positive.
When I first saw this result, I sent a message via our patient portal asking rheumatology if this could be done. I was told no. If they don't believe this to be a true positive, why not ensure that's the case? I wasn't offered any explanation.
Rheumatology is putting a lot of stock into the ANA titer. They have also encouraged us to start a medication that affects future ANA titers. Suppose Chloe has a low titer in six months because of rituximab therapy. Will her care be compromised because she still won't technically fit the criteria?
Without any other symptoms and/or lab abnormality, the investigation should not continue; this I agree with. There needs to be more than a positive ANA (regardless of titer) to go looking for something because pre-test probability matters. But that's not the case for Chloe. She was referred to a rheumatologist for a very particular reason: refractory ITP occurring at a very young age.
I admit I could be guilty of confirmation bias. But, rheumatology could be guilty of representativeness heuristic bias.
Although I made an entire case for SLE, it's not the question I need to be answered today. That diagnosis is nothing more than a label. It's a label that is hard to quantify because of how the clinical course for each patient varies.
There still is so much that needs to be known about SLE as we are limited by science. For this reason, the label is not the point.
Ultimately we want to know how this affects our daughter's quality of life long term. Suppose there will be deterioration or other organ involvement. How can we catch any changes as early as possible to prevent irreversible damage?
Unfortunately, most patients have organ damage by the time they are diagnosed due to the complexity of this disease. The terms "pre-clinical" or "incomplete" lupus are used for patients who don't technically meet the criteria but seem borderline. It's thought that treating at this stage can delay or prevent progression to SLE and subsequent organ damage. But how can this happen if we're dismissed and aren't even allowed to ask questions?
How many other parents are not allowed to have their voices heard?
I know my situation is not unique. I know our healthcare system needs change.
When the nurse practitioner called me, it was done without empathy or regard for our well-being.
She didn't acknowledge any of the abnormal lab results.
She didn't explain their thought process or even mention a plan for what we would do from a rheumatology standpoint.
They know that we saw every abnormality but did nothing to ease our minds. They recommended starting rituximab without any explanation of the risks. The medication was thrown our way as if it was no different than taking omeprazole.
There was no acknowledgment of the multiple visits we had to make to the hospital every week, where 10ml of blood was taken from our daughter each time.
I was livid. I don't have the words to describe what I felt. It was almost as if my daughter was nothing more than a test question, and the correct answer was (c) observe and follow up in 8 weeks.
But she's not just a lab result or a multiple-choice question. She's a human being who feels joy, sadness, and anger. As a parent, there isn't anything I wouldn't do to ensure the safety of my daughter. The stakes are high here.
Those in medicine often forget that you are dealing with the life of a human being. You are practicing medicine, but the outcome is someone's health and livelihood. Practicing medicine is beautiful; it should be honored and respected.
I asked questions and voiced my concerns mentioned above to the nurse practitioner, but I didn't get answers. I should rephrase that and say that I could have gotten better answers. To be frank, I don't know why she was the person following up when she wasn't the clinician we initially saw. She won't be the clinician we'll be following up with either.
I wasn't asking for the sake of being right. I was asking to be wrong.
I wanted someone to tell me why my concerns weren't valid. I wanted them to say confidently that nothing was wrong and that nothing needed to be done.
I didn't get that.
Instead, I was promised a follow-up call from Dr. "X" to address my concerns. It has now been one week, and we have yet to receive a call or even a message through the patient portal.
I have come to find that there are only a few pediatric rheumatologists at the hospital we're going to, and the rheumatologists aren't in the clinic every day because they are also working at another hospital.
When I discovered this information, some of my frustration shifted from the clinician to our healthcare system. The hospital is understaffed, and the clinicians are overworked. But it doesn't take away from the fact that they are still dealing with human life. They are also dealing with the mental health of two parents who desperately want to see their daughter healthy.
The decision to observe and start rituximab may have been the right one. Sometimes, we must give things time to see how they play out. But, the execution and communication were utterly wrong.
Unfortunately, the trust is gone.
I preach time and time again that lawsuits are not a result of a medical error. Medical errors happen all the time. Lawsuits typically occur due to a lack of communication before or after the mistake. Communication is the critical component here. No, I don’t plan to sue lol, I say that to make a point for every clinician reading this article.
Regardless, the hospital is understaffed, and my wife and I have decided that their rheumatology department isn't a good fit for our daughter. We have the resources and means to go elsewhere (something I'm incredibly grateful for).
I want to know that whoever sees my daughter isn't making a clinical error due to time constraints or burnout. I want to have my concerns heard and my questions answered. The good news is we didn't lose anything per se, as it took us weeks to complete the initial evaluation.
I've already set up an appointment to get a second opinion at Mayo Clinic next month in Rochester, Minnesota.
If you're a clinician, please remember that although you may stop thinking about the differential diagnosis for the patient in front of you after the visit, it carries on indefinitely for the patient (or parents in our situation).
Sometimes, the most important thing you can do for a patient is show you care.

As a nurse practitioner, mother of 5 and parent of a child who had a rare disease, I feel for you on so many levels. Knowing the limitations of the system gives you a leg up on the many patients in the system who don’t even know what they can / should question and at the same time leads you to demand that the system function at an optimal level for YOUR loved one (as you would hope it would function for everyone’s loved one).
Mayo has been the shining light at the end of the tunnel for many people I know, the labs there were able to give us the definitive diagnosis of anti-NMDAR encephalitis for our daughter. Ultimately after plasmapheresis, steroids, and IVIG didn’t clear her “mild” case, rituximab was needed. But even with advocating parents and on-the-ball clinicians, it was still a months-long process requiring multiple hospitalizations, time out of work, rehab and extreme emotional distress.
I hope your family gets the active listening and attention you deserve from your next team. Parents know their kids best. Wishing you luck in your search.
I hope she gets better soon but have sought any alternative advice. It’s hard when you work in med to think beyond the realm of prescription drugs but there are other viable options that may help. Wish her a speedy recovery & much peace mom/dad.